"I have a meniscus tear. Do I need surgery?"
I hear that question frequently. To answer it, lets briefly look at what the meniscus does.
The knee meniscus is a C-shaped structure made of fibrocartilage which functions as a shock absorber during daily activities. It is located within the knee between the top bone (femur) and the bottom bone (tibia). There, it not only protects the lining of the knee (hyaline cartilage) by its cushioning effect, but also protects the ligaments of the knee by acting as a stabilizer (see Figure 1). The meniscus absorbs up to 40-50% of the weight placed upon your joints so it is an important structure within your knee, and helps to keep it healthy. There are two menisci in each knee, one on the inside (medial), and one on the outside (lateral).
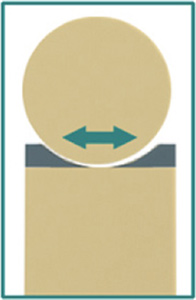
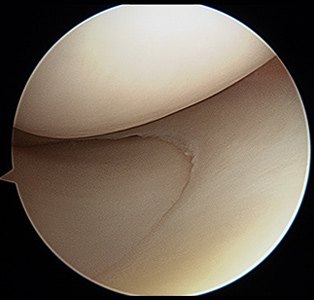
Figure 2 shows an arthroscopic view of a right knee medial meniscus. There is hyaline cartilage lining above and below.
Meniscus tears can occur by many different mechanisms. The first is the result of an acute injury, usually a vigorous twisting injury with the knee in a flexed position. These are often seen with athletic activities. Pain and swelling may occur soon after as well as difficulty walking.
A second mechanism of meniscus tearing is from minor trauma such as repeated squatting, kneeling, and twisting associated with daily activities. Pain and swelling may still occur but is usually less severe than that seen with an acute injury.
Meniscus tearing can also occur with chronic degeneration (arthrosis) of the knee. Much like a tire wearing out, the joint lining can wear out with the meniscus. Although there may be a minor injury which precipitates the problem, the wearing and tearing within the knee (including the meniscus) often occurs as part of a chronic process. Genetics and unhealthy lifestyle factors (overweight, lack of exercise, lack of sleep, poor nutritional choices) can lead to increased inflammation which further aggravates the joint breakdown.
Meniscus tearing can be strongly suspected based on the mechanism and physical examination. However, the diagnosis can be confirmed with MRI scanning, and I prefer MRI scanners with a power of at least 1.5-3.0 Tesla. This usually allows detection of meniscus tears quite accurately.
Once diagnosed, then what? The answer… it depends. Each person is different, and it is important to individualize a treatment plan which is specific to the patient, considering age, health, specific injuries, and desired activity/athletic goals.
Meniscus tears can occur with many different tear patterns and locations within the meniscus itself. Generally speaking, if the meniscus appears to be fully functioning and the tear is stable (no catching, locking, or popping) and is in a safe location, then I may consider an individualized goal-oriented physical therapy program, activity modifications, and gradual resumption of full activities as symptoms improve.
Most degenerative meniscus tears associated with chronic joint wearing are initially treated with a carefully applied arthritis treatment program including goal-oriented physical therapy, activity and lifestyle modifications, and occasional injections when appropriate.
However, if the meniscus tear is blocking the knee or interfering with its ability to act as a shock absorber, I may consider surgical options.
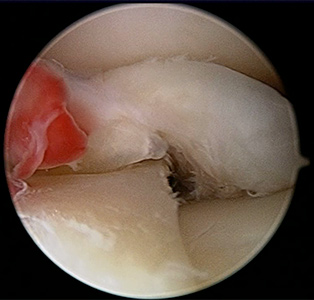
Figure 3 shows an arthroscopic view of a meniscus which is blocking the knee joint.
Meniscus surgery is done arthroscopically through a few small incisions. If the meniscus tear is seen to have poor tissue quality not amenable to repair, I will usually trim the smallest portion necessary to retain as much function of the meniscus as possible. Patients are allowed full motion and early weight bearing.
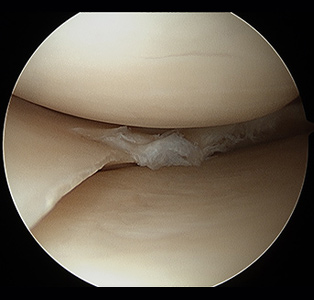
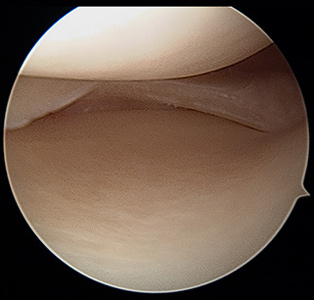
Figure 4 shows a small medial meniscus tear with poor tissue quality, and Figure 5 shows the remaining meniscus after the torn portion as been removed.
There is much scientific evidence supporting the benefits of meniscus repair on improving the shock absorbing, stabilizing, and joint protective functions of the meniscus. So, in general, if meniscus tissue is reasonable quality, for almost all tear patterns, especially in healthy younger patients with good surrounding cartilage, I will perform an arthroscopic repair.
This means the meniscus tear is carefully brought together and multiple sutures are passed above and below the meniscus and tied in the back of the knee to secure the repair. This allows early knee motion which supports the healing process. In complex situations, I will occasionally utilize additional biologic treatment within the joint to help stimulate meniscus healing.
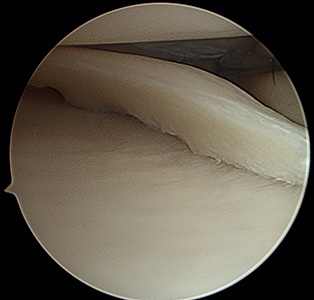
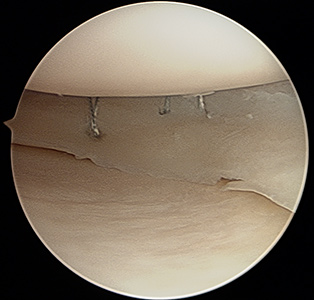
Figure 6 shows a bucket handle medial meniscus tear before repair, and Figure 7 shows the meniscus repair after sutures have been placed.
Depending on the meniscus tear pattern, there may be weight bearing restrictions up to four to six weeks. This protects the repair and improves the probability of restoring long term meniscal function.
For more details on meniscus tears watch this video.